
However, it should be recognized that radiographic evidence of joint injury is not perfectly correlated with the degree of arthritis pain and disability. Radiographs are relatively insensitive to joint changes during early OA, but are more accurate for the assessment of advanced OA. Weight-bearing radiographs with knee flexion provide better imaging of articular cartilage than non–weight-bearing images or those with the knee fully extended. Erosion and cysts of bone underlying articular cartilage are also common findings.
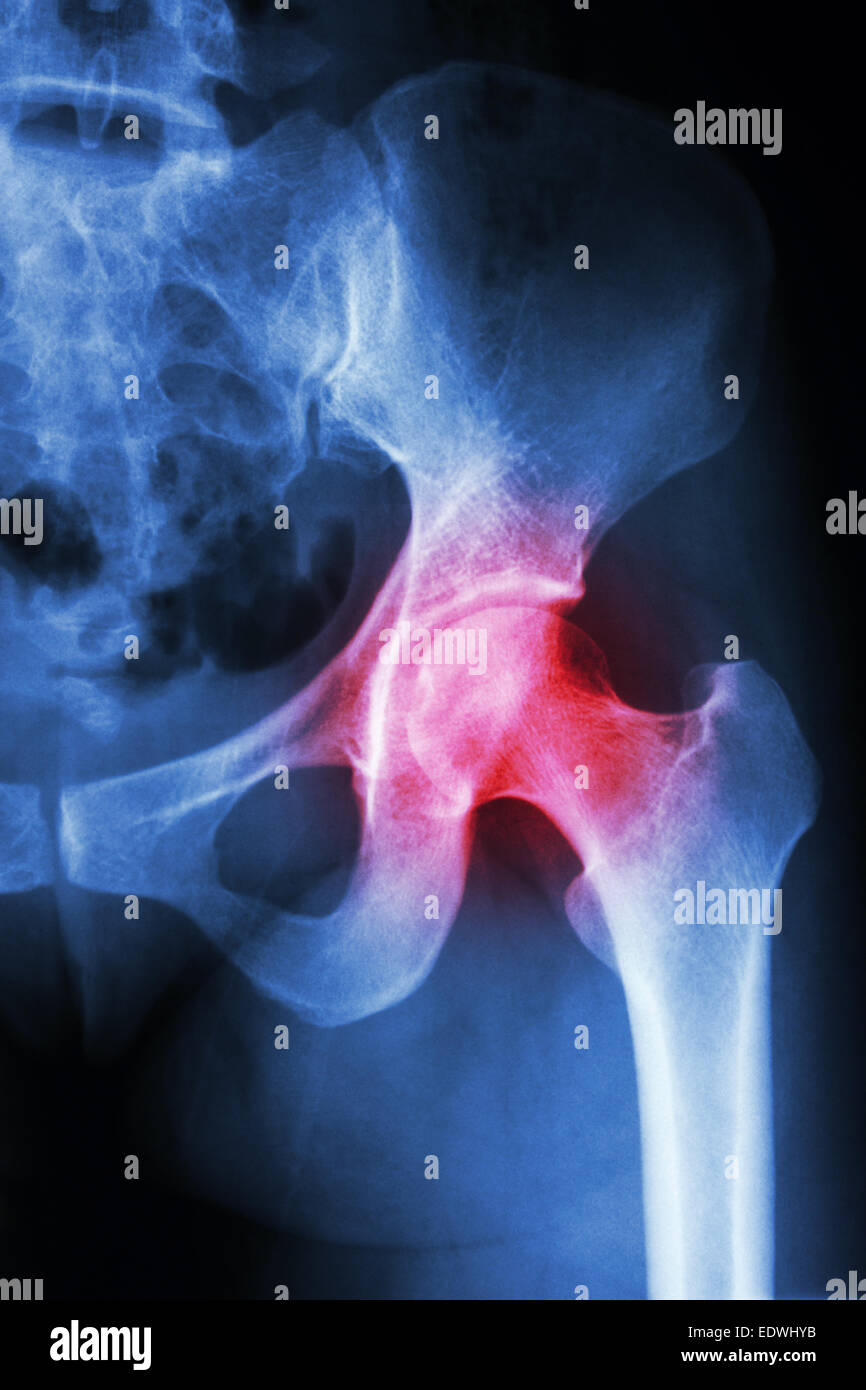
Radiographic hallmarks of OA include narrowing of the joint space that correlates with the loss of articular cartilage, increased bone density (sclerosis), and bone spurs.
According to guidelines for imaging patients with or suspected to have OA of the hip and knee, radiography is the imaging method of choice for OA assessment. Over time, patients with OA exhibit progressive degeneration of joint cartilage and the formation of bone spurs (osteophytes), as well as pathology of other tissues surrounding the joint. The pathophysiology of OA is not completely understood, but is thought to involve a multifactorial process that includes chronic inflammation, biomechanical stressors, and genetic predisposition. OA can affect any joint, but is especially common in weight-bearing joints, such as the hips and knees. Osteoarthritis (OA) - also referred to as degenerative joint disease or degenerative arthritis - is the most common type of arthritis and the most common chronic condition affecting the joints. More than 50 million Americans have some type of arthritis, with about 40% of these individuals experiencing arthritis-related activity limitations.
